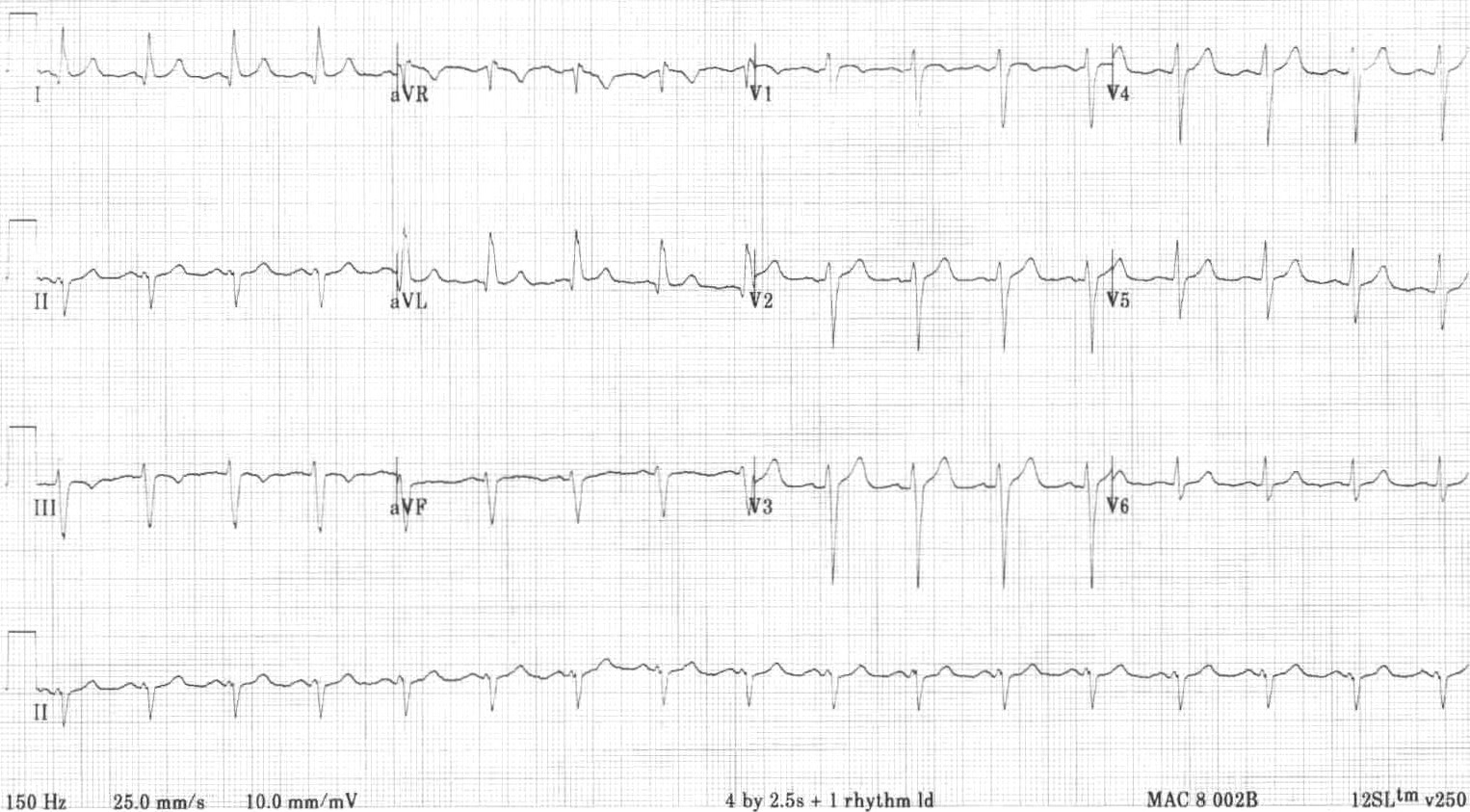
But you'll have a third wire connected to the left side of your heart so the device can keep both sides in proper rhythm. Left Bundle Branch Block LBBB - normal direction of septal depolarisation is reversed. This treatment is similar to having a pacemaker implanted. Sometimes this pattern occurs in atrial septal defect and it is known as crochetage sign. In addition the ECG also shows an intraventricular conduction defect (IVCD) in the form of notched R wave in lead II and aVF and an rSR’ pattern in lead III.

Such conduction delays may be due to myocardial fibrosis, amyloidosis, cardiomyopathy or hypertrophy. If you have bundle branch block with low heart-pumping function, you may need cardiac resynchronization therapy (biventricular pacing). This occurs when the focus is in the low atrium (low atrial rhythm or coronary sinus rhythm). Some patients develop nonspecific intraventricular conduction defects without any change in their QRS appearance. Such conduction disturbances may also be superimposed on existing bundle branch blocks and alter their appearance. Left bundle branch block (LBBB), right bundle branch block (RBBB), and non-specific IVCD were associated with increased mortality especially in patients with myocardial infarction (MI), , and heart failure (HF), ,.
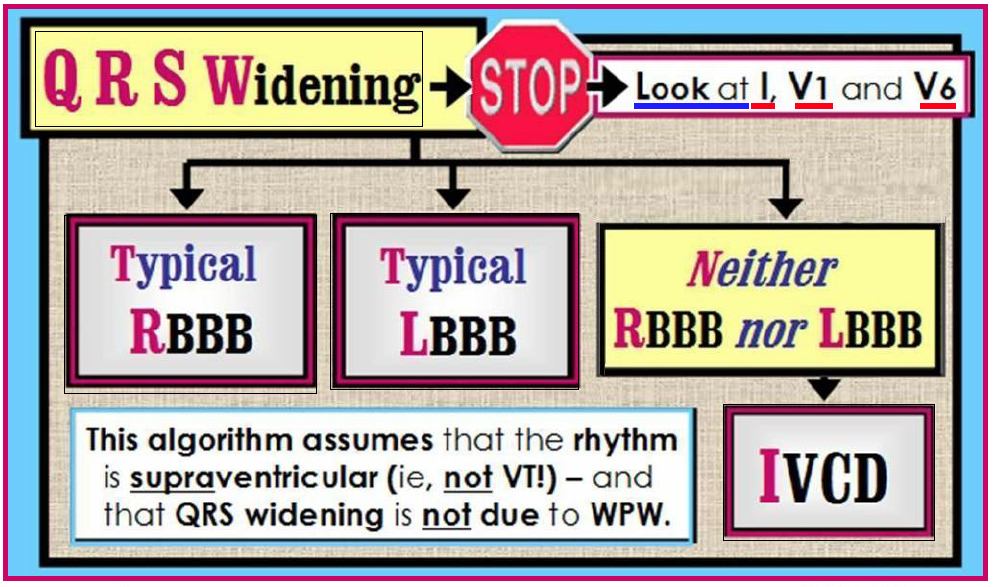
These conduction delays may be observed after large myocardial infarctions, in which the large necrotic area may cause nonspecific conduction disturbances. Intraventricular conduction delays (IVCDs) have been associated with impaired prognosis in patients with known cardiac disease. Definition and causes of nonspecific intraventricular conduction delayĪccording to the American Heart Association/American College of Cardiology and the Heart Rhythm Society (AHA/ACCF/HRS) recommendations (2009), nonspecific intraventricular conduction delay is defined by “a QRS duration greater than 110 ms in adults, greater than 90 ms in children 8 to 16 years of age, and greater than 80 ms in children less than 8 years of age without meeting the criteria for RBBB or LBBB.” At baseline, 1789 (15.1) patients had left bundle branch block (LBBB). Thus, the appearance of nonspecific intraventricular conduction delay may be rather nuanced. Nonspecific intraventricular conduction delay exists if the ECG displays a widened QRS appearance that is neither a left bundle branch block (LBBB) nor a right bundle branch block (RBBB). but intraventricular conduction delay (IVCD) with intact.

In conclusion, LVCD, whether LBBB or L-IVCD, was strongly associated with increased mortality in patients with and at-risk for CVD.Nonspecific intraventricular conduction delay conduction leading to left bundle branch block (LBBB) pattern (4). One historical presumption of LBBB has been that the underlying pathophysiology involved diffuse disease throughout the distal conduction system. After adjustment, LBBB and L-IVCD were similarly associated with increased all-cause (LBBB: 2.3, p = 0.001 L-IVCD: 4.0, p 120 ms) and CVD status. Left bundle branch block (LBBB) is associated with improved outcome after cardiac resynchronisation therapy (CRT). BACKGROUND Left bundle branch block (LBBB) is associated with atrial fibrillation (AF) and systolic heart failure, which can be treated with cardiac resynchronization therapy (CRT) that includes an implantable cardiac device (ICD). Study patients were 63 ± 9 years, 64% female, 75% Caucasian, 23% with established CVD. Adjusted Cox Models Adjusted for Baseline Factors Wald c2 P HR 95 CI Arrhythmic death or cardiac arrest IVCD 7.29 0.0069 1.44 (1.11,1.88) LBBB 4.22. Of 24,081 patients randomized, 22,067 (92%) were included with follow-up 34 ± 13 months. The primary outcome was adjudicated all-cause and cardiovascular (CV) mortality. IVCD was subclassified if left ventricular conduction delay (LVCD) was present (L-IVCD) or absent (O-IVCD). The researchers devised a first-of-kind subclassification scheme for IVCD. IVCD was defined overall as QRS 101 to 120 ms irrespective of morphology, or as QRS > 120 ms not identifiable as BBB. QRS duration was classified narrow (≤100 ms) versus prolonged (>100 ms) with additional categorization into left (LBBB) or right (RBBB) bundle branch block or nonspecific intraventricular conduction delay (IVCD). LBBB and RBBB were identified according to standard definitions (QRS duration > 120 ms). Patients with centrally adjudicated, nonpaced baseline ECGs were included. A post-hoc analysis was performed of the randomized-control PRECISION trial. We aimed to compare clinical outcomes of narrow versus prolonged intraventricular conduction on ECG stratified by QRS morphology and cardiovascular disease (CVD) status. The prognosis associated with prolonged intraventricular conduction on electrocardiogram (ECG) remains uncertain.
